大师访谈:Carpentier教授谈人工心脏瓣膜的发展
点击:6537次时间:2016-06-03 15:20:36


上世纪60年代早期,心脏外科迎来了曙光,外科医生治疗瓣膜疾病唯一的工具是Starr-Edwards的机械瓣膜,一种由美国外科医生Albert Starr 和工程师Lowell Edwards联合设计的 “球形”瓣膜。这种人工心脏瓣膜挽救了成千上万的患者,但缺点就是会形成凝血块。我记得有一位患者,是一位画家,我的导师Charles Dubost帮他做的手术,虽然他活下来了,但是一辈子和他脑部形成的血栓作斗争。
“我们救了他,但是我们并没有给他想要的生活”
这位患者最终瘫痪并且没有办法再绘画了。我们救了他的生命,但是没有达到他想要的生活质量。那时我决定寻求一种解决瓣膜疾病中血栓形成的方法。
神奇的不会形成血栓的移植物
我偶然知道一位伦敦的医生Donald Ross,使用人尸体的主动脉瓣膜作为移植物,并且没有血栓形成。这也许是我一直寻找的解决办法。
当我开始从尸体上收集瓣膜时,我发现它们常常受到感染。有种解决办法是在消毒的条件下使用猪瓣膜,此方法已经被牛津大学的Carlos Duran用于实验。可是他最终由于免疫排斥反应放弃了。我决定采用化学的办法来处理瓣膜,这样患者可以避免承担服用免疫抑制药的风险。
发现戊二醛可以消除免疫反应并且增强组织韧性。这就是生物瓣膜的概念
对组织进行处理而不是对病人进行处理是一个革命性的理念,在提供一个全新的视角的同时也带来挑战,需要比我过去在医学院学习到的更丰富的化学知识,因此我每周用两天的时间会去自然科学系学习,同时在实验室进行自己的研究。 我试验了不同的化学物质,如汞盐或甲醛,用来消毒瓣膜和去除组织抗原性,但它们都不成功。无数种的化学物质被尝试过,其中戊二醛被证明是最有效消除免疫反应和增强组织稳定性的物质。
从猪瓣膜到牛心包瓣膜:瓣膜的生物工程学设计
消除免疫反应的问题被解决之后又有新的问题被提出来:猪瓣膜的解剖结构不容易植入人体的主动脉瓣口,二尖瓣位置更不可能。把瓣膜放置到半刚性的支架中,这个难题就被很好地解决了,这样医生也能像植入机械瓣一样简便地植入生物瓣膜了。经过化学处理和安装支架,瓣膜不能再被叫做异种移植物了。所以我提议叫做“生物瓣膜”,这既显示了它的生物来源又说明了它的假体性质。“和移植物不一样,生物瓣膜的耐久性取决于经久不衰的化学处理后材料的稳定性和防止了宿主细胞内生”。
最近,带支架的概念有了新的运用,使得Alain Cribier发明的经皮导管瓣膜移植(TAVI)的发展具备了可能性。这是非常具有前景的微创技术。
意料之外的长期钙化
在猪瓣膜问世七年之后,没有想到的一个并发症是年轻病人开始出现钙化。这令人很诧异,因为我们只预期到延迟免疫反应或者组织退变。我返回到实验室,发现了一些会造成钙化的因素:病人的年龄和组织的化学组成成分,主要是微小钙蛋白和脂蛋白。我们试验了一些化学成分,通过减少磷脂来减轻钙化和消除微小钙蛋白。从爱德华方面来说,他们尝试了一些额外办法来保证疯牛病时期组织材料的消毒性。Aws Nashef也使用了各种表面活性剂。对我个人而言,我发现表面活性剂吐温80可以减轻钙化。这个发现引领了第二代生物瓣膜的发展,让生物瓣膜的耐久性从12年又增加了3到4年。
符合生物力学工程学的瓣膜:PERIMOUNT
另外一个问题是如何设计能够解决猪瓣膜无法满足各种大小人瓣膜的问题。使用牛心包瓣膜可以解决这个问题,牛心包瓣膜具有一些重要的特性,更规则的瓣叶,易于缝合到支架上,以及不同尺寸的可用性。
另一个优势是支架不仅能够支撑组织,而且还可以最大化减少钙化,因为在结合处向外弯曲支架10°,这样结合处就不会直接暴露在血流中而产生湍流--另一个加速钙化的原因。
ThermaFix处理:第三代生物瓣膜
此外,另一个进步是降低钙化,这是我的妻子Sophia做出的贡献,她第一个提出了在固定过程中加热戊二醛。为了最优化这个过程,找到最合适的温度和固定时间,需要无数次的实验。这是第三代生物瓣膜发展中最重要的一步,它至今还在临床上广泛使用。在大部分大于35岁以上的病人当中,瓣膜的耐久性达到了16年以上。
永远都有可能性
“这个并不是终点”。我们还面临着低龄化患者产生钙化的挑战,尤其是生物瓣膜可以避免抗凝药物的使用从而提高了生活质量,而这点对儿童来说获益更多。这个挑战需要我们不断地研究努力,永远都有向前一步的可能性。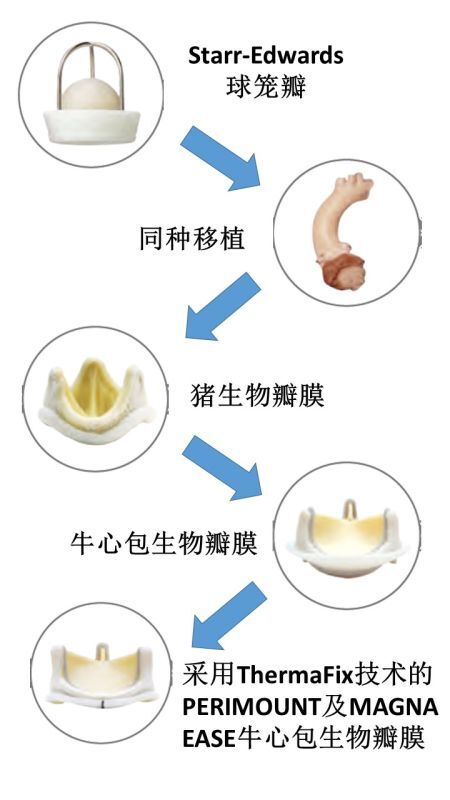
Ref:
Carpentier A: Lasker Clinical Medical Research Award. The surprising rise of
non thrombogenic valvular surgery. Nature Medecine 2007;13,10:17-20.
THE DEVELOPMENT OF THE VALVULAR
BIOPROSTHESIS
Alain Carpentier, MD, PhD
In the early ‘60s, at the dawn of cardiac surgery, the only tools the surgeons had at their disposal to cure valve diseases was the Starr-Edwards mechanical valve, a “ball valve” designed by the American surgeon Albert Starr and the engineer Lowell Edwards. This prosthesis saved thousands of patients but was confronted to clot formation. I remember a patient, an artist painter, who received such a valve from my mentor, Professor Charles Dubost. The valve saved his life but triggered the formation of a thrombus which migrated to his brain.
“We saved his life, but we didn’t give him the life he wanted”
The
patient became paralyzed and couldn’t paint anymore. We had saved his life, but
not restored the quality of life he wanted. At this very moment I decided to
work on the problem of clot formation in valvular disease.
The surprising non-thrombogenic power of grafts
I got to learn that Donald Ross, a surgeon in London, had used an aortic valve retrieved from a human cadaver, a homograft, without observing clot formation. It could be the solution I was looking for.
As I began to collect homograft valves from cadavers, I found that they were often infected. A solution could be to use valves collected from pigs under sterile conditions as already been tried experimentally by Carlos Duran in Oxford. Unfortunately, he had abandoned its use because of graft immunological rejection. I decided to confront this new problem by chemically treating the valve rather than the patient so as to avoid the burden and risks of immunosuppressants, an approach opposite to the current one.
Finding that Glutaraldehyde reduces immunological reaction and enhances tissue resistance. The concept of bioprosthesis
Treating the tissue rather than the patient was a revolutionary concept. It opened new perspectives but new challenges as well. They required more knowledge in chemistry than that I had acquired in the past at my Medical School. To increase my background, I decided to spend two days a week at the Faculty of Science and in the mean time, to develop my own research laboratory. Different chemicals were tried such as mercurial salts or formaldehyde to sterilize the valves and to reduce the antigenicity of the tissues. They proved unsuccessful. Numerous other chemicals were tried. Among them, glutaraldehyde was found to effectively reduce immunological reaction and enhance the stability of the tissue.
From Porcine valve to Bovine Pericardium:
Engineering the valve design
The problem of immunological reaction having been solved, a new one arised : the anatomy of the pig valve made it difficult to implant this valve in the native aortic valve orifice and impossible in the mitral position. This could be solved by inserting the valve in a semi rigid stent which could be implanted by the surgeon as easily as a mechanical valve. So chemically treated and mounted into a stent, the valve could no longer be called a xenograft. I proposed the term “bioprosthesis” which indicates its biological origin and its prosthetic fate. “As opposed to a graft, the durability of a bioprosthesis relies on the unfailing stability of the chemically treated material and the prevention of host cell ingrowth”.
More recently the stented concept found a new application in making possible the development of the transcutaneous valve implantation (TAVI) by Alain Cribier, a promising non invasive technique.
An unexpected long term calcification
Seven years after the introduction of the porcine valve bioprosthesis, calcification of the tissue emerged as an unexpected complication in young patients. This was a surprise because we rather expected delayed immunological reaction or tissue degeneration. I went back to the laboratory. The factors favoring calcification were identified: the age of the patient and the chemical compounds of the tissue, namely calcaphil proteins and lipoproteins. Several chemicals were tried to mitigate calcification by reducing phospholipids, and eliminating calcaphil proteins. On Edwards side, adjuncts were tried to secure the sterility of the tissue in a time where mad cow disease was a concern. Various surfactants were used in this aim by Aws Nashef. On my side, I found that the surfactant, tween 80, did mitigate calcification. Those discoveries led to the development of the so called 2nd generation bioprosthesis which added three to four years durability to the valve up to 12 years.
Biomechanically engineered valve: PERIMOUNT
Another issue was the unique size of the pig valve confronted to the various sizes of human valves. This was solved by proposing to use calf pericardium. The pericardial valve has several important features, more regular leaflets, easier suturing into the stent, and availability in different sizes.
Another advantage is the fact that the stent could be designed not only to support the tissue but also to minimize calcifications, at the commissures by bending the struts 10° outward so that the commissures being not directly exposed to the blood column do not generate turbulence, a factor of calcification.
ThermaFix Process : The third generation bioprosthesis
Another step forwards in calcium mitigation was a contribution of my wife, Sophie, who first proposed to heat the Glutaraldehyde during fixation. Many experiments were necessary to optimize this process, finding the optimal temperature and the optimal duration of fixation. This important step led to the development of the 3rd generation bioprosthesis which is clinically used today with an enhanced durability up to 16 years or more in most patients above 35 years of age.
It Is Always Possible
“This is not the end. We still have the challenge of calcification in young children, a particularly regrettable challenge because of the quality of life provided by a valvular bioprosthesis, which avoids the use of anticoagulants, would be specialy beneficial to children. This challenge requires our continuous effort of research. In research, it is always possible to make a step forward”.
Ref: Carpentier A: Lasker Clinical Medical Research Award. The surprising rise of non thrombogenic valvular surgery. Nature Medecine 2007;13,10:17-20.

